Residency Program Structure
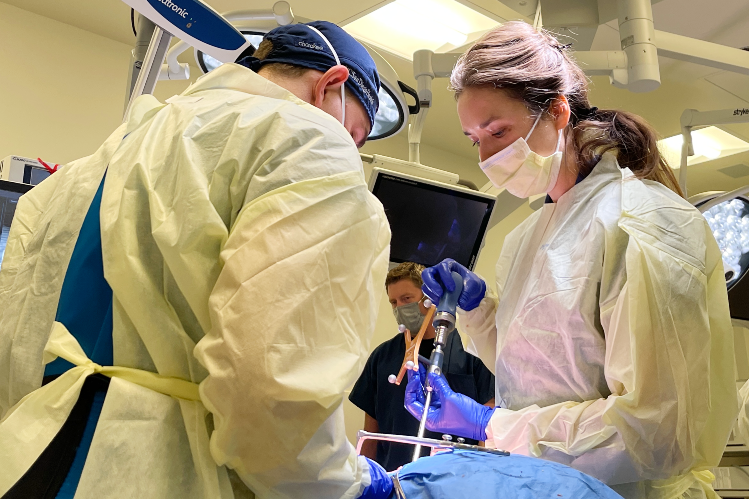 UC San Diego Neurological Surgery selects new residents for training each year. This seven-year residency (including internship) provides comprehensive training in all aspects of modern neurosurgery including neurosurgical critical care, neurotrauma, neurovascular surgery, brain tumors, functional neurosurgery, epilepsy, pediatric neurosurgery, peripheral nerve, and spine/spinal instrumentation surgery. The program is academic in its orientation, with input from world-renowned basic science researchers from the UC San Diego School of Medicine, UC San Diego Main Campus, the Scripps Research Institute, and the Salk Institute. The residency program is designed to be flexible and strives to accommodate specialized research and/or clinical interests.
UC San Diego Neurological Surgery selects new residents for training each year. This seven-year residency (including internship) provides comprehensive training in all aspects of modern neurosurgery including neurosurgical critical care, neurotrauma, neurovascular surgery, brain tumors, functional neurosurgery, epilepsy, pediatric neurosurgery, peripheral nerve, and spine/spinal instrumentation surgery. The program is academic in its orientation, with input from world-renowned basic science researchers from the UC San Diego School of Medicine, UC San Diego Main Campus, the Scripps Research Institute, and the Salk Institute. The residency program is designed to be flexible and strives to accommodate specialized research and/or clinical interests.
PGY-1
Neurosurgery, Neurocritical Care, Neuroendovascular
During the first year, interns spend six months on the neurosurgery service. Residents rotate at both the Jacobs and Hillcrest Medical Centers where they gain competency managing the neurosurgical inpatient census. This role includes critical bedside procedures, such as external ventricular drains and lumbar punctures.
PGY-1 residents also function as the primary consult resident for in-patient neurosurgery where they learn how to appropriately triage acute trauma, emergency room, in-patient, and community transfer consults.
Per ACGME guidelines, the remaining six months are divided among the neurocritical care (NCC) service, neuroradiology, neuropathology, and endovascular neurosurgery. All of these services benefit from world-class faculty who provide direct instruction and supervision of neurosurgical trainees. These interdisciplinary efforts are reinforced with shared didactic conference schedules.
As an NCC resident, interns collaborate with rotators from anesthesiology, neurology, interventional radiology, and internal medicine residents to care for critically ill patients with a range of neurologic and multisystem injuries. As neuroendovascular residents, interns learn the procedural principles of diagnostic angiography and are exposed to management of various neuroendovascular pathology, such as large vessel occlusions, aneurysms, dissections, and vascular malformations.
PGY-2
Junior Neurosurgery Resident
The second and third years of the program concentrate on developing skills in basic neurosurgery and neurosurgical critical care. Introduction to operative techniques commences with rotations on both the Tumor and Spine services, providing dedicated study in fields within neurosurgery in order to allow residents to develop mastery in these areas. This includes endovascular neurosurgery exposure, neuroradiology, and neuropathology as well as six months spent at Rady Children's Hospital on the Pediatric Neurosurgery Service.
The PGY-2 resident in neurological surgery has a unique opportunity to develop specific skills related to neurosurgery. The resident will focus on developing their skills in the operating room setting amongst the range of nuanced neurosurgical procedures.
Every day is spent in the operating room learning the basics of spine, cranial, and vascular surgery while simultaneously supervising and teaching the intern floor and ICU management of neurosurgical patients. Time in the second year is divided evenly between the La Jolla service and the Hillcrest service providing time on a busy elective operative service and a busy trauma center.
During the PGY-2 year and thereafter, evaluations will occur on a semi-annual basis using the six core competencies developed by the Accreditation Counsel of Graduate Medical Education (ACGME). These reviews further include academic productivity and resident case logs. Particular emphasis will be made on assessment of appropriate goals within the competencies with specific emphasis on those areas, which are particularly important to the training of a highly competent, empathic neurological surgeon with optimal clinic and intellectual skills.
PGY-3
Junior Neurosurgery Resident
The PGY-3 year is divided evenly between the La Jolla service and the pediatric neurosurgical service Rady Children's Hospital. Particular emphasis of the six months at Rady Children's will be placed on the development of skills in the performances of procedures unique to the pediatric age group including shunting of low birth weight infants, the correction of new spinal dysraphic states, the performance of surgical procedures for tumors primarily found in the pediatric age group, and the correction of craniofacial disorders.
The remaining six months are spent with the La Jolla service continuing to work on a busy quaternary service including spine, oncology, vascular, and functional neurosurgery.
Residents will continue to develop increasing skills in the acquisition of medical knowledge, patient care, a commitment to lifelong practice learning and improvement of communication skills with patients, families and other health care professionals.
Residents enjoy opportunities to learn more about medical ethics and the need for a commitment to lifelong professional development. The program also provides exposure to different systems of practice beginning at UC San Diego Hillcrest, Thornton / Jacobs Medical Center, and Rady Children's Hospital, which are unique environments with different structures of resident functions and systems of care.
PGY-4 and 5
Research/Elective
UC San Diego has one of the highest-ranked neuroscience research programs in the country. The presence of the Salk Institute, Scripps, La Jolla Institute for Immunology, and a robust biotechnology sector make San Diego a truly unique and world-class environment for research, career development, and innovation.
The fourth and fifth years of neurosurgical training involve protected research or an enfolded fellowship. During this time, residents have the opportunity to perform either clinical research or participate in a basic science laboratory. At this time, residents will have significant exposure to biostatistics and biomedical ethics.
Most residents choose to spend two years participating in research, and take advantage of this unique environment to further neurosurgical care and uniquely position them for careers in academic medicine.
Residents must take and pass the in-service training written examination in neurological surgery prior to assuming the clinical duties of the PGY-6 year. Should a resident not pass the examination, a dedicated education plan will be developed to ensure appropriate educational support and success.
PGY-6
Neurosurgery Senior Resident
Six months of this year will be spent as the senior resident on the complex spine service utilizing the University Hospitals and the Veterans Administration Hospital. The VA provides valuable training both in the operating room and in the clinic setting for surgical decision making. During this rotation, residents gain exposure to both EMR and CPRS medical record keeping systems. The experience of running the Neurosurgical service adds to the resident experience in administrative, leadership, and teaching responsibilities at the VA.
Six months of the PGY-6 year is spent as the chief of the pediatric neurosurgical service at Rady Children's Hospital. Experience in this high-volume, largely complex cranial practice provides further microsurgical training on a wide array of complex tumor and vascular cases.
The combined rotations of the PGY-6 year serve as an important lead up to the final year of residency by allowing for significantly increased operative and clinical decision-making independence, but also in managing a multi-disciplinary team and training junior residents.
Chief Year
The resident will serve as chief resident during the seventh year, the busiest and most highly rewarding year. Six months is spent in La Jolla at the Jacobs Medical Center and six months at Hillcrest, our Level I Trauma Center, where the chief has additional responsibility for managing resident clinics.
The chief resident year provides the opportunity to demonstrate the capabilities of clear and independent decision-making. This is a demanding position that requires both surgical excellence and strong leadership.
The program's objective is to expose the chief resident to the most complex and demanding operative situations. Chief residents are also expected to provide a significant educational role for the junior residents in regard to neurosurgical procedures and clinical care.
Special emphasis will be placed during the evaluation of the chief resident's final year on their skills in teaching, communication, and professionalism in addition to the basic requirements for technical and clinical excellence. In 2020, both residency program graduates finished with more than 2,200 cases.
